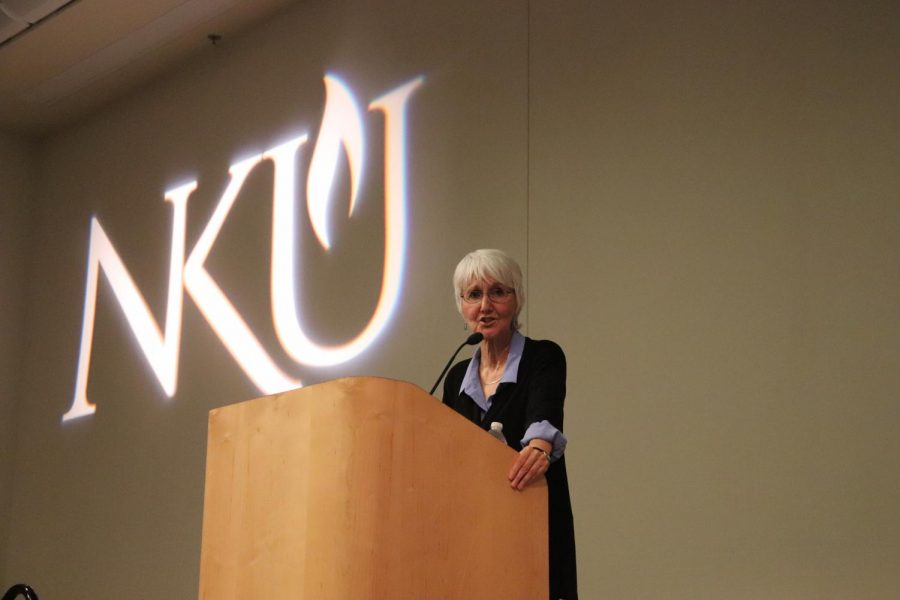Your donation will support the student journalists of Northern Kentucky University. Your contribution will allow us to purchase equipment and cover our annual website hosting costs.
A conversation with Sue Klebold, mother of Columbine shooter
The Northerner sat down with Sue Klebold, mother of Dylan Klebold, and asked her about self-care, mental health and more
October 11, 2019
Sue Klebold, mother of Dylan Klebold, spoke to NKU students, staff, faculty and community members about mental health.
Content warning: This article addresses topics of suicide, mental health and mass shootings.
Sue Klebold—mother of Dylan Klebold, one of the two gunmen responsible for the Columbine shootings—spoke with The Northerner Wednesday morning. Klebold spoke to NKU students, staff, faculty and community members Wednesday evening as part of an event series for Mental Health Awarenesses Week.
The Northerner: This year was the 20th anniversary of Columbine and in your memoir, at first, you mentioned that you and your family pushed the press away. What made you decide to start telling your story and talking about Dylan?
Sue Klebold: “What made me decide to do that was the fact that I’ve been working on a book for so many years; I actually had been working on this book for 15 years. And I knew that as a condition of sharing my story, I would have to meet with the media. So that was something that I had to decide that I would do and not be afraid. But the actual sharing of my story was something that I had to begun to do in very controlled settings long before the book came out. I was beginning to speak at suicide prevention conferences, violence prevention conferences because I felt that people told me that when they knew my story, they they would parent differently—they would be more alert, they would be more perhaps intrusive in some cases. So I decided that maybe it would be beneficial for people to hear the story. And that was part of what helped me do that. And also, it gives me a way to remember my son and have his life, not be about just the way he died and try to do something in his memory too, and in the memory of everyone who was killed, who died, who was hurt.”
RELATED: Reaching for hope: Mother of Columbine shooter shares her story
N: On the website for your book it says all the author’s profits are going to a mental health organization. Can you talk to me about that decision?
SK: “I knew that, as the mother of a killer, I could not and should not benefit in any way from the sale of this book. And I felt that I had things to say that might be important for people to hear. And I didn’t want their thought that I was profiting make them not buy or read the book. So I wanted to just remove that as an obstacle because I thought it would just—might encourage people to read it, who might benefit from it. And I just had this feeling in my heart of what was ethical and what was not. And it did not feel ethical in any way to take money for the publication of that book. So I didn’t.”
N: In other interviews, you’ve said that, in retrospect, your son showed suicidal behaviors and thoughts? How has shedding awareness on mental health helped you process what happened at Columbine?
SK: “We have a very difficult task when we talk about mental health and violence because we know that people who have a serious diagnosis of a mental health disorder are no more dangerous than anybody else. With that being said, I believe that people get into a state where their mental health is deteriorating, but they do not have a diagnosis of a serious mental illness. And that is a growing number of people. And in that, counseling departments all over the country—in the world—even can verify that. And what I believe was that when I looked at how Dylan could be there, and he was such an unlikely person to ever hurt anyone, I had to try to examine how he came to be there doing what he did that day. And as I did that, and I examined and considered the fact that he was suicidal, and that his own suicidality played some role in his being there. What I really learned is that, certainly planned mass violence incidents, the individual goes through a process of deterioration, and suicidality is usually a part of that. And so that’s why I want to talk about that—this difficult line of trying to understand what a mental illness is versus what mental wellness is. And I believe that my son was not mentally well. They have certainly done some studies with brains to show that people who have died by suicide have differences in their prefrontal cortex. So I really believe that, at the time of his death, he didn’t have access to choice the way we do when we’re in balance. And that’s sort of where I’ve been trying to spend my time try to understand.”
N: You’ve obviously done countless interviews. But what’s one specific question or topic that media outlets don’t typically ask you that you wish you could talk about more?
SK: “You know, I cannot answer that because I feel over time I have been asked everything that I wish I’d been asked. Perhaps, if there is one thing, I want people to feel empowered … to know what we can do when our own thought processes feel different to us, to know how to get help, where to get help? So I think the thing that I would wish people would understand is that there are things we can do to try to mitigate our persistent thoughts. Maybe we may be having suicidal feelings of being preoccupied with death, whether it’s harming ourselves or harming someone else, that isn’t necessarily something we have to listen to and pay attention to, as if we have no choice—that this is a progression. There’s intervention that is possible, there are helping, there are things that can be done to mitigate and help the person. And I think that’s one thing that’s probably most important message of all that I wish everybody would ask.”
N: What role do you think that institutions should play in intervening in mental health, like NKU, or high schools?
SK: “I think everybody has a role to play, not just higher-ed institutions. K-12 does, the medical system and that’s huge chunks—there’s emergency, there’s primary care, there’s mental health system. I think everybody has a role to play. And what I see happening is, there are really two things that I think very simply branches out. When I have had worked with suicide loss survivors, they kind of fall into two categories. In one group, there are those of us who had no idea that the individual was suffering, no idea at all. Didn’t know what signs to look for, didn’t know that the person could possibly be thinking about that. Yet they died. The other group has some knowledge that their loved one is struggling. And they’re on a downward spiral. Maybe they’ve been hospitalized, beat rehab, whatever it is, yet, they still lost that individual. So what I see very clearly is that it that kind of leads the way for society, we have to educate ourselves, our families, so that we know how to interact with our friends and our loved ones and ourselves—to listen to ourselves. That’s a huge piece that universities and everyone else can do. And the other piece is when they do get to help, how is the profession, and the professions, that helped this person helping them live. Universities play a role because not only are they caring for their own students, but they are educating the professionals of tomorrow. And so I think, you know, better counseling and support services, better opportunities for connection. But in addition to that, really looking at the curriculum and finding out in education, in healthcare in counseling, are there suicide prevention components to that training, for example? And so those are just the two major huge pieces without getting too specific.”
N: As you repeatedly speak on the issue, in particular, the events of that day, how does that affect you personally?
SK: “Talking repeatedly about that day and the effects of that day is still traumatizing for me. When I do presentations such as this, I actually have a recovery period and when I do a presentation, I have to make sure that I have downtime. Just to give an example, I recently did an event that I had multiple things in a day and a half, I had to give three speeches and two, you know, press conference and when I got home, I was unwell. I could tell that because I was having nightmares about my son. And, so, like everything, like all of us, we have to practice self care, and I think can’t be masochistic in doing this work, I have to back away from it and realize that I do have a personal life, and to dwell in that place where I am safe and hopeful and comfortable. I can’t spend all of my time doing that because it’s just too painful.”
N: How do we deal with the stigma that mental health and mental illness face all the time?
SK: “It’s a huge problem. And it is often a barrier to getting help. And I think the only way to get past that is what we are currently trying to do. You’ll see a lot of people who have struggled with mental health symptoms come forward and talk about it. This is why I’m here because not only did my son take part in a mass violence incident, but in the aftermath of that I had, you know, acute anxiety disorder … when we experience bad feelings, when things aren’t working right in our thoughts, we not only have those feelings, but we have feelings about those feelings. So it creates this vicious circle that if we don’t have hope, if we don’t have a sense of ‘this is a temporary condition, I’m having a bad day,’ then whatever that condition is worsens. I think one of the ways to combat stigma is to help people understand that when we go through these things that this is a period of time. It’s like having a tendon that’s in pain. You know you’re going to be struggling with it, or wearing a boot for eight weeks or whatever. To help us understand that there are things we can do to help ourselves feel better. And to learn how to help each other, to learn how to recognize in ourselves what the signs are, that we’re not well. All these things have to happen.”
N: What is your go-to tactic for self care? What’s the number one thing you do to take care of yourself?
SK: “I think the first important thing is to listen, to try to be perceptive enough to what’s going on. The way I do it is through quiet. I do yoga; I do exercise. I connect with people, friends, friendships, love, walks, hobbies, I do art. These are things that make me feel connected to a larger world. But I still think the most important thing for us is to stop scurrying around, to sit quietly enough to really sense what is going on with us.”
N: When you were writing your memoir, what was the biggest struggle that you faced when you’re writing it?
SK: “I think the biggest struggle I faced was knowing that somewhere at the end of this pipeline, I would have to become public—that I couldn’t publish a book and still hide. Because it was so much more comfortable for me to hide. Yet I had a story that I wanted to share and I needed to share. I had a mission of teaching because I had been a teacher. And that eventually overrode any the reservations that I had. But I was writing this from the moment it happened because I’m a journaler and I was writing everything that happened in those 15 years. The writing of the book was easy; it was natural. But the toughest thing was to realize that at the end of that I would have to put a face and a name and be public. And that was not so easy.”
Suicide prevention resources
If you or someone you know is having thoughts of suicide, there are resources available near you:
National Suicide Prevention Lifeline: 1-800-273-TALK (8255)
Crisis Textline: Text CONNECT to 741741
Health Counseling and Student Wellness Crisis Line: (859) 572-7777
University Police: Call 911 or (859) 572-7777
National Alliance on Mental Illness Kentucky Crisis Line: (800) 950-NAMI (6264)
To schedule a counseling appointment at Health, Counseling and Student Wellness: (859) 572-5650